First Aid for Equine Emergencies
We never want to see our beloved horses hurt, but sometimes it happens. Prepare before anything happens with a first aid kit for horses, a treatment plan, and skills to administer first aid for equine emergencies. Many healthcare decisions can be made before an accident, saving further stress and heartache. Emergencies are a tough pill to swallow but need planning.
TABLE OF CONTENTS
Treatment plan and end-of-life plans
It’s always best to have your horse’s medical history available in an emergency, as well as major decisions made, before the emergency.
Medical history and vital signs
- While it’s absolutely fabulous that you have your horse’s entire medical history memorized, it needs to be in a location that is readily accessible if you are not. Barn managers, vets on call, and anyone helping your horse should be able to find and understand your horse’s history.
- One option is an online data management program for barns that track training, appointments, and diets. Written notes in a binder are another. However you decide to keep the history, make it accessible to those needing it.

Some vets have access to your horse’s history while on the road, but they still need details of daily life.
Your horse’s medical history
- In some horse emergencies, it’s helpful for the treating vet to have more information. Log dates and details about:
- Vaccines
- Deworming protocols
- Medications
- Diet and access to pasture
- Feeds and supplements
- Allergies
- Any known injuries
- Known disorders, especially metabolic disorders
- Quick access to your horse’s vaccine information is essential to forming a treatment plan in some cases. Wounds may need a tetanus booster, exposure to wild animals may require a rabies booster, and eating moldy hay may influence the need for a botulism vaccine.
- Past fecal egg counts and deworming protocols are valuable to know when evaluating a colic case, as are diet changes and the types of feed and supplements your horse eats.
- It all works together to give your vet a holistic picture of the many variables that often accompany an emergency.

Do not share with your roommate, no matter how annoying they are.
Vital signs
- Your horse’s vital signs – temperature, pulse, respirations, gum color, capillary refill time, and digital pulse should be predictable when your horse is at rest. Changes to vital signs mean something – the importance of which may vary.
Ranges of horse vital signs
- For basic TPR – here are the expected values for horses. These measurements are at rest – meaning your horse is calm and collected, not immediately after a ride or playing in the field.
Temperature:
- A horse’s normal temperature varies from 99.5º to 101.5º F. For foals, up to 102º F is normal.
- Use a digital or non-mercury shake-down thermometer to take your horse’s temperature. Add some lubrication like jelly or KY or even A & D ointment. Digital thermometers will measure temperature quickly and beep when finished. Shake-downs take longer, but there’s no battery, which at some point will come in handy.
Pulse
- For the pulse (heart rate), expect to find 24 to 40 beats per minute, although most horses are between 32 and 36 beats per minute. For newborn foals, 80 to 100 is normal, and for older foals, 60 to 80 is normal.
- You can easily take your horse’s pulse with a stethoscope, wedging the diaphragm behind the left elbow. Stethoscopes also come in handy when listening to gut sounds – another “normal” you should know about your horse.
- Alternatively, you can find the artery that crosses your horse’s jaw bone and press down about halfway. For either method, count the beats for 30 seconds and multiply by two.
Respirations
- Respirations per minute are typically 8 to 12. For foals, count on about 60-80 breaths per minute.
- Count your horse’s inhales and exhales as one breath. Observe and feel along your horse’s flank, which roughly lines up with the ends of the lungs. You can see and feel your horse’s lungs expanding the flank.
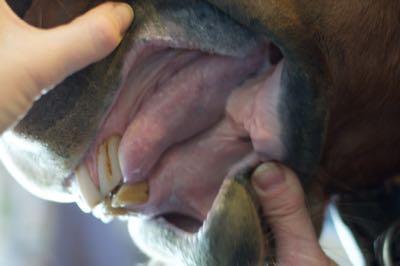
Gums
- Your horse’s gums should be pink and slippery. Dry or sticky gums indicate dehydration. You can also monitor your horse’s gums with the capillary refill test. Press your thumb into the gums above the front, upper teeth for a moment. The gums should turn white under pressure from your thumb. Count the time for the white thumbprint to return to the usual pink color; it should be about 2 seconds for the gums to return to the starting color.
Gut sounds
- The symphony of sounds your horse makes while digesting his food is one more way to keep tabs on his health. Ideally, you have a good idea of his gut sounds on a typical day.
- Those gut sounds give your vet valuable information about what happens in each part of the digestive system during colic. It’s useful information when you can tell your vet which quadrant doesn’t sound the same.
How to find the gut sound locations
- The best spot for gut sound listening is around your horse’s flank, where the hair grows up. There’s an upper and lower portion on both the right side and the left side, making up the four quadrants.
-
- The upper left corresponds to the small intestine, which is typically pretty quiet.
- The lower left corresponds to the large intestine.
- The upper right reflects the cecum and large intestine.
- The lower right side is the large intestine.
- As you listen for gut sounds, keep your ears peeled for bubbles, a few of which happen every minute. You may also hear groans, which usually occur every few minutes. Your horse tells you something is wrong when these sounds change or disappear.

The digital pulse
- Taking your horse’s digital pulse can help give you an idea of what’s happening inside the hoof. The digital artery delivers blood to the hoof and the digital vein brings it out of the hoof. If there is swelling inside the hoof, the vessels inside the hoof have a more challenging time moving blood. The artery will pulse and throb as it works harder to pump blood into the hoof.
- When looking for the digital pulse, it’s a good thing if it’s missing or faint. A stronger or bounding pulse indicates inflammation inside the hoof, which usually pairs with pain.
Finding the digital pulse
- To find your horse’s digital pulse, run your fingers down the leg tendons. Follow them as they wrap under the fetlock. In that area, you should find a soft spot. If you press into that spot and run your fingers side to side, you feel the digital artery and vein, rather like guitar strings. If there is a pulse, you will find it by pressing it down halfway. Pressing too much will stop any pulse.
Treatment and end of life plans
- Making tough decisions in horse emergencies is a horrible experience, so try to make as many beforehand. Some things to consider:
- Decide when your horse trailers to a hospital for treatment or surgery. Work with your vet to outline circumstances that warrant a trip to the hospital.
- Make general decisions about what types of surgery your horse could go through. Some horses may not fare well with colic surgery, so it’s helpful to have guidelines.
- It’s essential to understand the costs of surgery, hospital trips, and alternatives like euthanasia. Euthanasia is a kind gift to give your horse, and you may have options as to after-care. Know the options in your area and their costs long before you decide. Also, know the protocols at your barn around this procedure and where it can happen.
More about the emotional decisions that can be made ahead of time here.

When to call the vet
- There are two general reasons to call the vet:
-
- Your horse’s vital signs are off. Keep in mind that wonky vital signs may mean your horse is sick, or he just ran 29 laps before you showed up. Context is key, so look for other big-picture clues.
-
- When in doubt, call the vet!
A quick list of emergencies that you may encounter:
-
- Colic
- Laminitis and any hoof pain
- Sudden or severe
- Street nails
- Choke
- Bleeding – from the nose, on the legs, anywhere really
- Diarrhea and other changes to the manure
- Any foreign body – don’t take it out!
- Active labor for 20 minutes without progress
- Any eye injury or change to the eye
- And any changes to your horse’s vital signs and behaviors. Does this mean you need to call the vet if his temp is a little high? Probably not if he’s been running like a fool in the pasture and it comes back to normal.
- Any changes you find to something specific, like vital signs, are noteworthy. But – look at the big picture and notice behaviors, reactions, movements, the situation, and attitudes.
Specific equine emergencies to prepare for
Colic
- Hopefully, any instances of colic with your horse are mild and vanish quickly. But it’s hard to determine possible outcomes just by your horse’s behaviors. Some colics seem relatively mild and end up in surgery. Other cases look horrific, and one hour later, nothing is wrong. Avoid judging books by covers here.
Know the signs of colic:
- Pawing. You may find your horse pawing at the ground or track marks in his bedding or the paddock footing.
- Circling. Like a dog just before he lies down, horses seek relief from the pain by circling. Maybe they lie down or are just agitated and need to move around.
- Looking at the flank. It might seem like your horse is actually staring at his belly and flank as if to say, “what is going on back there.” Indeed – what IS going on?
- Belly kicking. This often looks like a horse kicking at flies, and sometimes he’s just trying to get relief by jostling his insides.
- Stomping. Another indication of colic pain that resembles annoying flies.
- Higher pulse rate. Pain creates a measurable response in your horse’s vital signs. A higher resting pulse rate, and sometimes respirations, indicate discomfort.
- Excessive sweating. Too much sweat is another sign of pain somewhere in your horse.
- Going down and getting up repeatedly. This up-down cycle is your horse looking for comfort.
- Not eating or drinking. Many horses will never turn down food and water, even during extreme emergencies. When that desire is gone, it’s a red flag.
- Changes to your horse’s manure – Do you notice fewer manure piles than usual, a different consistency, a change in fecal ball size, dry or watery fecal balls, or your horse’s choice of location has changed? All red flags.
- Changes to your horse’s urine output. Many horses will assume the posture to urinate when colicking. Some will frequently urinate in small amounts to relieve pressure in their guts.
- Flehmen response. While this upper lip flipping is usually associated with enhancing interesting smells, some horses use this gesture to indicate discomfort.
- Abnormal or absent gut sounds help narrow down the source of any colic discomfort.

Just rolling or colic?
When you first notice the signs of colic
- Contact your vet for instructions. Avoid the “wait and see” approach – which causes some problems. First, pain meds interfere with the diagnostic process. And, if you are waiting and nothing changes, your horse has spent that much more time hurting when your vet could have been heading to you.
- Only give meds if instructed. Describing your horse’s condition to your vet before they arrive will give you a preliminary plan, including the need to walk, any pain meds, and the proper dosage.
- Remove food from your horse. Colic disrupts the digestive system, and if something is clogged, twisted, or bloated, adding food compounds this problem.
- Keep him comfortable and safe. A horse violently tossing about a stall is likely safer in a larger paddock. If your horse is in the blazing sun during summer, moving to a shaded location may help him be more comfortable.
- Add bedding, usually. There are some cases in which suspected colic is actually laminitis, and soft bedding will help ease the hoof pain. More shavings will help soften the impact of repeated rising and going down in colic situations.
- Walking should be case-dependent. There is little science that indicates walking a colicking horse is helpful. More often than not, valuable energy needed for healing is wasted on walking.
- The importance of a rectal exam. While colic is not an actual diagnosis in and of itself, it can lead to twisting of the gut. A rectal exam by your vet does a few things. Your vet can feel possible twists, which gas colics can cause. Impactions may also be felt, which helps in the formation of a treatment plan.
Things to tell your vet about colic:
- All vital signs. Give your vet your horse’s vital signs with comparisons to the norms. This lets your vet know just how “off” things are.
- Digital pulses are essential for monitoring for a few reasons. Colic and laminitis can look the same. Colic can also lead to laminitis is the disruption to the digestive system, and the microbes within become unbalanced.
- Any differences you hear in each belly quadrant.
- Changes to inputs and outputs. Describe any variance in your horse’s eating, drinking, peeing, pooping. Changes may include frequency, volume, texture, location, and any other unusual indications.
- Let your vet know about any lifestyle changes your horse has experienced. Is his training or turnout plan different/ Has he gone to shows, clinics, or been stressed at home?
- Know when the last fecal egg count and deworming protocol were done. Internal parasites are one reason that horses colic.

Diarrhea
- While colic is a catch-all for all things that upset the digestive system, look for diarrhea. Watery manure and diarrhea may seem transient, and it might well be. But, diarrhea in horses can be the result of lots of things:
-
- Sudden change in food, hay, or pasture.
- Snacking on toxic plants
- Various horse diseases, like Potomac Horse Fever, that are contagious to other horses
- Colitis, an inflammation of the colon
- Problems with water re-uptake in the digestive system
- Intestinal parasites
- Cancers
- Inflammatory bowel disease
- Salmonella bacteria
- Sand overload in the belly
- Obviously no horse is going to be comfortable with diarrhea. Is the cause something benign, or are further complications on the way. And certainly, if there is a contagious disease floating around the barn, it’s time for isolation procedures.
- Dehydration is certainly a side-effect of diarrhea in horses. While some horses may need some extra water in their meals, others need IV treatments. The most concerning complication upsets the intestinal microbes. These guys are sensitive to changes, and a die-off or imbalance creates toxicity that easily ends up in the blood and the hooves – enter laminitis.
Laminitis
- Laminitis can, unfortunately, take the life of a horse. Sometimes this is swift, and in some cases, can drag on for months and years.
- Once a horse starts to show signs of hoof discomfort, getting your vet and farrier to help your horse is essential. Abscesses, bruises, fractures, and laminitis can all look the same. Your vet needs to examine, diagnose, give pain medications, and create a treatment plan. Your farrier is there to help execute the treatment plan and support the hooves in the healing process.
Signs of laminitis
- Horses will often start feeling hoof pain for hours or days before it’s evident to you. Early signs of laminitis are vague and often mimic other hoof problems. Laminitis signs to notice:
- Is your horse sore after a farrier visit? Sub-acute laminitis cases often experience soreness after a trim or shoeing. Sometimes, the trim is too short, creating bruising. If the trim is appropriate and soreness exists, this is something to investigate with your vet.
- Hesitancy walking – You may notice that your horse acts as if walking on eggshells. Tender-footed steps may be more evident on harder surfaces, and some horses will hesitate before moving from a soft surface to a hard surface.
- Turning is difficult for the horse with laminitis. It may seem like he is hopping sideways to avoid twisting the lower limbs. A laminitic horse may also take many tiny steps to maneuver around.
- Colic-like signs are sometimes evident in laminitis cases, as horses are seeking a new position to get relief from the hoof pain.
- Changes in posture are typically thought of as a horse stretching the front leg(s) out and rocking back on the haunches, but it’s only seen in about 25% of cases.
- Warm or hot hooves indicate pressure and swelling inside the hoof. This heat usually pairs with increased digital pulses. Digital pulses are more telling, as measuring heat in the hoof is subjective and may be because a horse was standing in the sun.

Equine first aid for laminitis
- Calling your vet is the first thing to do. Laminitis can go sideways faster than you can blink – early intervention gives your horse the best chance at recovery. Your vet can then help you develop an immediate care plan.
- Only give medications for pain relief after talking to your vet. As with colic, pain meds may interfere with the diagnostic process.
- Then make your horse comfortable. The softer his footing is, the better his hooves will feel. You may not want to walk him from the back pasture to the barn, so perhaps bring bedding to him.
- Keep his water close to limit how much movement he needs to do for a drink.
- Remove grains, supplements, pasture, treats, and anything high carb or high sugar. Many horses with laminitis have a direct link between diet and metabolic diseases like pituitary pars intermedia dysfunction (PPID) and equine metabolic syndrome (EMS). Insulin resistance (IR), another risk factor for laminitis, can be a component of EMS and PPID. With these metabolic disorders, the sugars in your horse’s diet need to be rare.
- Ice those hooves! Ice is an effective and inexpensive way to decrease painful swelling. If possible, ice the lower legs to cool the blood as it enters the hoof.
- Reduce any stresses that your horse may be experiencing. Make sure he can see friends, have easy access to water, and feels safe in his stall. Your vet may advise you to allow slow feeding of his regular forage, helping to keep his mind occupied.
Street nails
- Street nails are a slang way of describing a foreign body in the horse’s hoof. Foreign bodies in the hoof is an emergent situation, and needs careful handling to minimize the risk of complications. When a horse steps on a nail, screw, or anything that penetrates the hoof, you must talk to your vet before you do anything.
- Foreign objects in the hoof can damage the laminae, the joints, the coffin bone, the bursa near the navicular bone, any tendon or ligament in the area, and more.
- The second wave of danger is the puncture that the street nail creates. This opening is the perfect location for bacteria to develop a raging and painful infection. Infections in the hoof are difficult to treat – Medications are hard to deliver, and horses stand in dirt, shavings, manure, urine, and all sorts of infection-causing stuff.
What to do about street nails
- Generally speaking – don’t remove any foreign objects until your vet can take x-rays. Radiographs give your vet an idea of the damage inside the hoof.
- Very rarely will you find a street nail that is partially embedded. In cases like this, your vet can tell you what to do. If additional movement pushes the object further into the hoof, your vet may want you to remove it. However, do everyone a favor, take photos of the entrance location, and mark the object’s depth with a pen once you have it removed. Also, mark the location of the puncture. Pictures help, too. This is all risky business, and your vet needs to be involved.

I found all of these in a pasture.
Treatment for street nails
- Sometimes, surgical intervention is needed, as well as preventative measures to ward off infections. Special shoes, called hospital plates, cover the sole and can be moved to apply medications. The goal is to keep bedding, manure, urine, footing, and everything else out of the channel.
- Pain management is paramount, too. The hoof’s internal structures are all contained in a mostly inflexible capsule. As swelling increases, the pain inside the hoof increases as it has nowhere to go.
- Take preventative measures against laminitis. When a horse’s leg is severely injured, the partner leg takes the brunt of your horse’s weight. The strain can lead to supporting-limb laminitis in the healthy hoof. This may be a slowly developing problem, and diligent monitoring, preventative icing, and anti-inflammatories are helpful.
Leg wounds
- Leg wounds run the gamut between a tiny scab and non-stop bleeding when it comes to leg wounds. Generally speaking – your routine should be:
-
- Stop bleeding (if necessary)
- Clip
- Clean
- Consult with your vet
- Cover
- Maybe a standing wrap
Minor leg wounds
- Smaller wounds where the bleeding has stopped are usually found when grooming – you may feel a little scab or swelling and heat in the area. You may also notice some hair loss or a trickle of blood. Just because a wound is small doesn’t mean it’s minor.
Clip the wound
- The best way to treat a tiny wound is to clip the hair around it. Clipping allows you to see the harm clearly, prevents hair from interfering with healing, and you can efficiently apply medications.
- If the wound is open, and there’s a good chance that clipped hair will fall into the wound, so prep the area. Use some water-soluble jelly, like KY, to coat the wound. When you rinse it off after clipping, any stray hairs and dander go with it.
- Use trimmer or body clippers to clip a wound with a clean and sharp blade. For best results, use a #30 or #40 blade, as these remove quite a bit of hair. You can use your #10 or something similar, but there will be longer hair on the edges.

Clean the wound
- There are three good options for cleaning wounds, saline, chlorhexidine, and betadine. It’s tempting to use hydrogen peroxide or rubbing alcohol – but these are irritating and can cause more tissue damage.
- Saline is probably your best bet and much better than what comes from the hose. If you have some, flush the area, and you are done.
- Chlorhexidine is that blue, anti-microbial cleanser. Use it diluted, about an ounce per gallon of water. You can rinse the wound first, then rinse again with a chlorhexidine dilution.
- Betadine can be found as a solution (diluted) or as a scrub. Your choice! Rinse the wound, then dab some betadine on the area. The scrub version will foam a bit. Rinse away any residue. There could be some distinct yellow-orange staining on lighter coats.
Consult with the vet
- Now that everything is tidy and clean, decide if your vet needs to take a look – either by photo or an in-person visit.
- Your vet will decide if sutures are necessary, it largely depends on how many layers of tissue are involved. Wounds on or near joints and moving parts may open, and sutures can complicate healing.
The chance of punctures
- The problem with puncture wounds is their initial appearance as a small and superficial nick. The outer wound will close easily and quickly, leaving a tunnel that traps and incubates bacteria – the beginnings of an infection.
- Punctures on the legs are especially problematic as they can penetrate tendons, ligaments, and joints. There’s no easy way to spot a puncture unless you can pull something out – which is a questionable thing to do anyway and should be treated like a street nail.
- Your vet can confirm a puncture by probing the wound, checking for depth with sterile tools and a plethora of anatomy knowledge and experience. Don’t play doctor in cases like this.
Cover the injury
- Keep the wound protected with some covering. Leg wounds are susceptible to the germs and dirt in bedding, turnouts, and any surface they lie or walk on.
- Using a topical medication or protective spray can help fight infection, too. There are many options out there – from fancy colored sprays, silver sprays, powders, creams, and ointments.
- You may want to avoid a topical treatment that dries (like spray or powder) around joints, as movement can crack any dryness. Creams and ointments are easier to wash away if you or your vet needs to recheck the wound.
Standing wraps
- There is always swelling and pain with wounds, varying with extent, location, and movement. Standing wraps serve two purposes for wounds – to reduce inflammation and protect the wound from dirt and shavings.
- There are two schools of thought out there about standing wraps when a singular leg is injured – do you wrap one or both legs? It’s likely not an issue to wrap both, especially if the injured leg takes less weight. But, for minor abrasions, wrapping the injured leg may be all you need. Your vet can advise you.
Actively bleeding wounds
- When a horse is still bleeding from an injury, do what you can to stop the bleeding.
- Use diapers, maxi-pads, cotton rolls, cloths, or whatever you have in your horse’s first aid kit to apply pressure to the wound.
- Try and keep your horse calm as you grow another set of arms to apply pressure, help your horse, and call your vet.
Do not remove the bandage if your first layer of bandaging is soaked through. Add more layers of bandage on top and keep pressure applied.
- There is also a powder you can keep in your equine first aid kit that helps bleeding stop. Pour the packet into the wound and cover with pressure.
Swelling of the leg(s)
Tendon and ligament swelling
- It’s not always a torn tendon or ligament that causes swelling on the lower legs. Even small cuts and nicks can create inflammation.
- When you discover the swelling, cold hosing or icing will help reduce the inflammation and pain. There’s a chance that the injury will have icing as part of the treatment, so you might as well start early!
-
- limit movement
- cold hose or ice
- maybe standing wraps
- get the vet for an ultrasound and other diagnostics
- Depending on the severity of the swelling, you may want to limit your horse’s movement. Certainly, movement can help swelling decrease, but lamenesses may be exacerbated by activity. This is especially true with tendon and ligament damage.
- Ideally, your vet can see your horse as soon as possible. Lameness exams, bloodwork, x-rays, ultrasounds, and other diagnostic techniques can pinpoint a cause. But, more importantly, a treatment plan can hatch.
Excessive swelling
- If the leg(s) look more like stovepipes than actual legs, this is definitely an emergency. There are two things to be aware of, and each can happen in hours.
Cellulitis
- Phlegmon is a strange condition that most of us call cellulitis. When the cells just below the skin’s surface become infected, cellulitis happens. Cellulitis can be a superficial infection or can travel into muscles and tissue, often creating swelling in the entire leg.
- Something is wrong when you find a hot and swollen leg. The primary problems with cellulitis are:
-
- Quickly spreading infection
- Swelling to the point of lameness
- Skin stretching until it tears
- Damage to the skin if it sloughs off
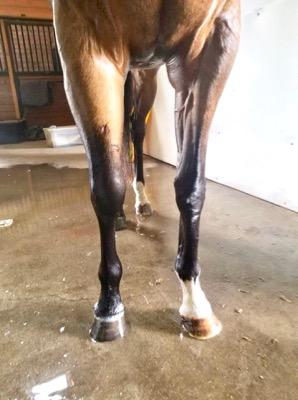
One of these legs is not like the others
Lymphangitis
- When the vessels of the lymphatic system become infected, lymphangitis sets in. The lymph system does not operate on a pump like the cardiovascular system. Instead, your horse’s muscles and movement pump the fluids and metabolites cleaned from the blood vessels.
- Permanent damage to the lymph vessels is possible, creating permanent swelling in the leg(s).
- You will notice swelling and heat. You may also find your horse has a fever, is painfully lame, and even acting colicky.
- Lymphangitis closely resembles cellulitis and your vet can help distinguish between the two. The treatments often involve lots of patience, antibiotics, wrapping, and movement. Ironically, the road to healing is LONG with these conditions, as the onset is quite fast.
Typical in-barn treatments for cellulitis and lymphangitis
- Your horse may need supportive care, such as:
-
- Ice, ice, more ice
- Poultice, in some cases
- Standing wraps
- Topical medications, if needed
- Stall rest sometimes
- Hand walking
- Oral antibiotics and anti-inflammatory medications
Splints
- Splint bone injuries, often referred to as “popping a splint,” teeter between totally benign and needing surgery. Your horse may or may not be lame, although most horses with a freshly popped splint.
- On either side of the cannon bone, the splint bone can get knocked, the ligaments under it can inflame, and the bone itself can break anywhere along the length. And these spindly little bones are longer than you might think.
- Some splints are never an issue and resolve themselves untreated. Others need rest, ice, wrapping, medications, and even surgery.
- A sound horse with a splint injury still needs the vet. Fractures may not produce lameness but can interfere with the tendons, ligaments, and surrounding structures.

This splint bone has a small fracture on the end of it where the splint bone has peeled away from the cannon.
If your horse “pops a splint”
-
- Cold hose or ice, you can do this 20 minutes at a time, with breaks in-between.
- Have your vet out for possible x-rays and a treatment plan.
You may also need to:
-
- Medicate
- Continue icing
- Poultice
- Stall rest
- Standing wraps and supportive care
Choke
- When a horse chokes, the food lodges in the esophagus on the way to the stomach. Choke in humans refers to a blockage of the airway. You may notice your horse:
-
- Stops eating
- Stretches his neck out
- Stands still when he should be eating
- Has drool from the mouth and/or nose
- Makes gagging sounds or other strange noises
- Tries to spit out food
- Choke is an emergency. Call your vet, even if you think your horse has cleared the blockage. Choke can cause damage to the esophagus, pneumonia, ulcers, and inflammation that increases the chance of a repeat episode.
Eye injuries
- There is only one thing to say about eye injuries: Eyes don’t grow back. Eye injuries are also excruciating. Call your vet if you see anything abnormal in, on, or around your horse’s eye, such as:
-
- A different or sudden eye discharge
- Closed eye
- Swollen eye area
- Cuts around the eye
- A different look to the eye – cloudy, shinier, just not the same
Look out for these behaviors, too:
-
- Unusual spooking
- Different stance to see things
- Rubbing the eyes on the legs
- Head tossing
- Flinching when you are around the face
- Many horses will quickly recover from eye injuries when promptly attended to. Per your vet’s instructions, pain medications are necessary, and you may be applying ointments every few hours.
- Provide your horse with a fly mask during healing. You could use duct tape on the fly mask to block light from the area over the injured side. There are specialty fly masks available for all sorts of eye injuries and conditions, too.

Nervous system issues
- You may find that your horse is showing signs of a neurological disorder. The signs of nervous system issues may come on quickly or take weeks and months to express fully. In either case, your vet needs to be the first call.
Signs that may indicate a neurological problem:
-
- Stumbling and uncoordinated walking
- Balance issues and lack of coordination in the head or legs
- Weakness
- Seizures
- Blindness – full or partial
- Unusual behavior – circling, pawing, pacing
- Head pressing
- Twitching and muscle spasms
- Lack of appetite
- Lethargy
And the list is long of possible culprits:
-
- Injury
- Botulism
- Poisoning
- Autoimmune disorders
- Tetanus
- Ticks
- Abnormal metabolic functions – thyroid, sugar levels, etc.
- Blister beetles in hay
- Some neurologic disorders can swiftly debilitate and cause death. Others may be managed over time but may pose injury hazards if coordination problems create falling.
Urinary system problems
- You may find that your horse has strange behavior while urinating to trying to urinate. Bladder problems can escalate to bladder rupture. A horse’s stance, movements, frequency, volume, and consistency of urine can indicate problems. Problems with the urinary system are immediate emergencies.
Signs of urinary system problems in horses:
-
- Straining to urinate
- Unusual stance or posture while urinating
- Urine is dark
- Urine is otherwise different than normal with regards to volume, frequency, foam, and color.
- Horses with colic often urinate frequently in small amounts to relieve any pressure in the belly. While this may appear strictly a urinary system issue, it may be colic instead. Just another reason to call the vet!
- If you see any unusual urine or urination pattern, try and catch a sample in a clean and sealed container. Your horse may need a urinalysis, and sometimes you don’t have time to wait until the next time your horse urinates.

How well do you know your horse’s urine habits?
Respiratory problems
- Horses have lungs that span most of their giant bodies, and there can be things that go wrong with a horse’s ability to breathe.
- Heaves is a respiratory problem that is not necessarily emergent but can have episodes of excessively strained breathing that make it an emergency.
Sudden respiratory problems that send up red flags are:
-
- Strange nasal discharge
- Hyperthermia – overheating will certainly change breathing patterns
- Blood from the nose
- Unusual sounds, posture, head position, or changes to eating and drinking – is something lodged in the respiratory system?
- Abrupt loss of stamina
Hypothermia and Hyperthermia
- These two emergencies can have long-lasting effects and even death. When a horse’s temperature is below normal, it’s hypothermia, and overheating is hyperthermia.
- When the horse’s body temperature fluctuates in either direction, the best thing to do is call your vet. The horse’s brain becomes confused about warming and cooling in both situations, and full-body inflammation can happen. In a tidy little nutshell, both of these conditions can lead to organ failure and death.
The other pickle in this big dilemma is that some warming and cooling treatments can make things worse.

Keep taking your horse’s temperature, and log the time and values to track progress.
Hypothermia
- Rarely does a horse become so cold that its entire body drops in temperature – but it can happen. Horses cast in cold mud or in weather without fat, a wintercoat, and sometimes even a without a blanket are at risk of hypothermia.
- When a horse’s body temperature drops below about 98.6º, hypothermia begins. It can be mild, moderate, or severe, depending on how cold the horse becomes. Severe cases have temperatures below 82º.
The treatment for hypothermia depends on the severity.
- Mild cases may need blankets and shelter. More severe cases need fluids, lavage, or actively warming the horse with lamps and heating pads.
- These treatments can be risky and should not be done without your vet. Adding heat sources can often backfire, as the external heat warms the legs, pulling circulation from the core, where it’s needed most.
Hyperthermia
- Overheating in horses is dangerous. It’s nice to know your horse’s normal temperature at rest and after exercise and how long it usually takes to return to the normal temperature.
- When a horse’s body starts to warm up, it could tip above 105.8º and become heatstroke. Some fevers can create hyperthermia, often teetering dangerously close to this.
- As with hypothermia, the goal is to bring the body temperature down. While you are waiting for your vet, do the following:
-
- Get your horse into the shade
- Offer water
- Start logging times and temps, as well as other vital signs
- You may notice that your horse has stopped sweating – and typically, this means that his body has cooled. However, with hyperthermia, sweating can stop, necessitating the observance of temperatures with a handy thermometer.
- After talking to your vet, you may need to use cool water as a treatment. You can even drape towels on your horse to hold some cool water. Using cold water tricks your horse into shivering which naturally increases his body temperature, defeating the purpose.
- Your vet may also need to give IV treatments to aid in cooling and hopefully prevent any significant organ damage.
Make an equine first aid kit
- Knowing horses, a first aid kit is something you use more often than you would like.
- Many tools in your kit will come about as you need them and have to make a mad dash to the tack shop. Let’s hope that particular inconvenience is rare and you are stocked and ready. There are some essential items to have, and some extra items that may come in handy. You may also want to assemble a hoof first aid kit, too.

Recommended Equine First Aid Kit Contents
Essential Items:
Have the tools to monitor your horse’s vital signs:
- Thermometers are mandatory, and you have a few options. Digital thermometers are fast, but the battery can run out. A backup would be a non-mercury shake-down style.
- Stethoscopes are useful for taking your horse’s pulse and monitoring gut sounds.
Wound Cleaning
- Saline is a gentle and effective flush for wounds.
- Betadine comes in a scrub or solution formula.
- Chlorhexidine is another anti-microbial solution for wound cleansing. You can also use chlorhexidine to wash your horse’s grooming brushes. Dilute according to instructions.
- Blood stop powder is easily poured into wounds to help clots form.
Bandaging
- Diapers are great for bleeding and packing hooves.
- Non-stick bandage pads or maxi pads buffer the wound under a standing wrap. This also keeps any ointments or medications against the wound without messing up the bandages.
- Sheet cotton is used under bandages and tears easily for the perfect fit. You can use smaller pieces to cover minor wounds.
- Gauze wrap covers sheet cotton for use under another bandage or standing wrap. It’s flimsy and thin but secures any pads, cotton, or cushion before wrapping.
- Self-adhesive tape AKA Vetrap, but there are lots of other brands. There is some “give” to this wrapping.
- Elastikon tape is used when you need something covered for a long time. It’s super-sticky, even more so if you leave it in your car for a day.
- Electrical tape has stretch and is ideal for wrapping the top of bandages or standing wraps when the horse tries to pull off his bandaging.
- Spider bandages are great for covering joints. The arms of the spider bandage allow for a custom fit over knees, hocks, and any moving parts.
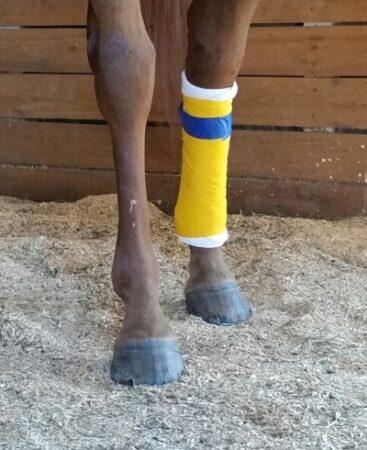
Your vet can help you decide if you need to wrap one leg or both.
Syringes
- 10 or 12 cc syringes are great for dosing most medications, orally or via injection.
- 60 cc syringes are handy dosing meds and flushing out wounds in weird places.
- Needles are necessary to draw up meds, then switch to a fresh needle before injection. Aim to keep two needles for every syringe if injections are something you are trained to do.
More essentials
- Bandage scissors for bandages and so much more. They have blunt ends for safety.
- Hoof pick with brush, because you can never have too many hoof picks.
- Show Touch Up spray is fabulous for marking your horse with your phone number in case of emergency evacuations.
- Pen and notepad offer a way to keep organized if you are medicating and rehabbing. Go charts and graphs!
- Flashlight, or better yet, headlamp for nighttime emergencies to free up your hands.
- Clippers for trimming wounds. If you want cordless trimmers, you need to have them charged all the time. Otherwise, opt for a corded set. Keep sharp blades on hand.
- Disposable gloves because horses can be gross.

Trimmers with this type of adjustable blade are great for equine emergencies and clipping wounds.
Go above and beyond your first aid kit:
- Ice packs and heat packs – to reduce swelling and provide pain relief. It’s helpful having boots or wraps that can secure them on your horse.
- Clay poultice provides cooling relief to the lower legs, but don’t use it over a wound. You will need to cover with newspaper or a feed bag liner before applying a standing wrap.
- Electrolytes are helpful in some cases, and paste is best for emergencies. Adding electrolytes to your horse’s feed won’t work if your horse can’t have food.
- Fly mask for eye situations.
- Clean bucket for diluting wound cleaners
- Twitch for emergency holding.
- Twitches have a limited time – you have about five minutes. Please don’t twitch unless you have been taught.
- Potential Medications to Keep on Hand:
-
- Dipyrone (Metamizole) – anti-spasmodic & mild analgesic.
- Banamine (Flunixin Meglamine) – strong analgesic & antipyretic.
- Bute (Phenylbutazone) – great anti-inflammatory.
- Your vet can give you detailed instructions about dosing and frequency. Also, note that some injectables can create severe side effects if given improperly. Flunixin and Phenylbutazone can be given orally in paste form to save everyone the trouble of needles and syringes.

Using twitches is a science, learn properly before attempting.
Hoof first aid kit
- Hooves are hardy structures – until they’re not. Hoof emergencies, and non-emergencies, often require some protection. It’s helpful to have boots and farrier tools before you are on the porch waiting for your newly ordered supplies.
- Sharpie pen for noting where street nails land, or for tracking the growth of cracks and other hoof defects.
- A system to ice hooves and lower legs for laminitis or laminitis-risk cases. For pain management and inflammation control, hooves can stay iced for days straight – yes, no breaks.
- Farrier tools for shoe removal, because horses don’t always want to toss the entire shoes; sometimes a tweaked shoe is in order.
- Hoof packing materials for all sorts of ailments.
-
- Poultice and Magic Hoof for soles.
- Epsom salt poultice for abscesses.
- Ichthammol and Sugardine for wounds.
- Some thrush-busting solution for those pesky infections, the green or purple stuff is a good start.
- Bags for soaking hooves in cases of abscesses or white line disease. You can also use an empty 5-L fluid bag if your vet shares with you.
- Epsom salts for soaking hooves.
- A hoof wrap for quick fixes if there’s a missing shoe, or when you need to hold some hoof packing in there.
- Sturdy hoof boots for whole hoof protection.
- Soft, supportive boots for horses with laminitis or who are at risk of laminitis.

This is one style of hoof boot to help with laminitis.
That should get you started! And most importantly – when in doubt, just call the vet.
Stock up here for your horse supplies! As an Amazon Associate, I earn from qualifying purchases, but it’s ZERO extra cents to you. You can also visit my Amazon storefront here: PEG storefront.
Every horse owner needs a digital thermometer for fast and accurate vital signs
Help your horse cool out in hot and humid weather.
Reliable wound gel from trusted horse peeps at Vetricyn.
If hooves are your jam, this book is for you.
For bits, sores, dry patches, cracked skin, and more. Great for your horse's first aid kit!
The gold standard for stinging hooves and anytime you need to pack the hooves.
Support and softness for laminitis and other painful hoof conditions.
This medical tape will quite literally hold your life together, it's that amazing.
Vetricyn's classic wound cleaner boosted up with a GEL formula! Perfect for defying gravity while caring for your horse's latest mystery ouchie.
Sticks to itself, not to your horse. Keeps the dirt out!
These boots are my favorite for wrapping hooves with poultice or clay and a diaper. No more duct tape boots! You can also use inserts with these for more squish.
These SilverSox are great for protecting the legs from rubs, help with scratches and mud fever, and provide some compression, too.
Take the heat out, reduce inflammation, help prevent long-term damage, and dress your horse in cute colors after a ride.
If hooves are your jam, this book is for you.
and adds a nice sheen!
A simple and trusted hoof supplement.
For added squish during laminitis or other painful hoof trauma.
The gold standard for stinging hooves and anytime you need to pack the hooves.
Hi-quality no-bows with Back On Track reputation (that's good!)
These boots are the gold standard for jumpers and horses that like to interfere.
Support and softness for laminitis and other painful hoof conditions.
Buy bulk and save! This is great for stubborn hoof infections like seedy toe and thrush.
These squishy quilts are the perfect mix of no-bows and thicker quilts.
Feed your horse's hoof health from the inside out.
This supplement helps high-laminitis risk horses and has calming ingredients like magnesium.
The gold standard for bell boots in a rainbow of colors.
Classic, clean, stylish boots for your horse. Great for jumping.
Be practical when wrapping your horse's legs with a traditional color, but toss in some spice with the understated pattern!
Protect your horse's legs and let them shine bright.
These boots are my favorite for wrapping hooves with poultice or clay and a diaper. No more duct tape boots! You can also use inserts with these for more squish.
This style is great to protect the hoof, but is not soft and squishy for laminitis cases.
Show off your horse's legs with these safe, reflective, and fashionable boots.
These boots are great for protecting barefoot horses.
These SilverSox are great for protecting the legs from rubs, help with scratches and mud fever, and provide some compression, too.
Simple! Easy!
Take the heat out, reduce inflammation, help prevent long-term damage, and dress your horse in cute colors after a ride.
These are amazing for riding. They take some wrestling to get on, but they will stay on.
Thank you!